Herniated disk: Difference between revisions
imported>Robert Badgett (New page: A herniated disk is defined as "an intervertebral disk in which the nucleus pulposus has protruded through surrounding fibrocartilage. This occurs most frequently in the lower lumbar regio...) |
mNo edit summary |
||
| (21 intermediate revisions by 3 users not shown) | |||
| Line 1: | Line 1: | ||
{{subpages}} | |||
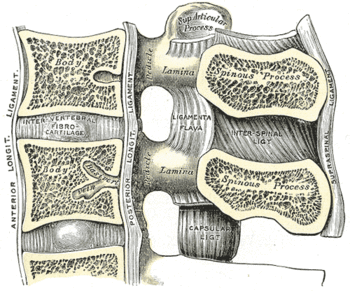
{{Image|Grays-image301.gif|right|350px|Median sagittal section of two lumbar vertebræ and their ligaments.}} | |||
In [[medicine]], a '''herniated disk''' is defined as an "intervertebral disk in which the nucleus pulposus has protruded through surrounding fibrocartilage. This occurs most frequently in the lower lumbar region.".<ref>{{cite web |url=http://www.nlm.nih.gov/cgi/mesh/2007/MB_cgi?mode=&term=herniated+disk |title=Intervertebral Disk Displacement |accessdate=2007-11-13|title=Intervertebral Disk Displacement |author=National Library of Medicine |authorlink=|coauthors= |date= |format= |work= |publisher= |pages= |language= |archiveurl= |archivedate= |quote=}}</ref> | |||
A herniated disk is an infrequent, but important cause of [[lumbalgia|low back pain]]. A herniated disk is more likely when [[sciatica]] is present. | |||
==Epidemiology== | |||
{| class="wikitable" border="1" | |||
|+ Prevalence of abnormal intervertebral disks of the lumbar spine in people without back pain.<ref name="pmid8208267">{{cite journal| author=Jensen MC, Brant-Zawadzki MN, Obuchowski N, Modic MT, Malkasian D, Ross JS| title=Magnetic resonance imaging of the lumbar spine in people without back pain. | journal=N Engl J Med | year= 1994 | volume= 331 | issue= 2 | pages= 69-73 | pmid=8208267 | doi=10.1056/NEJM199407143310201 | pmc= | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=8208267 }} </ref> | |||
! Abnormality!! Definition!!Prevalence | |||
|- | |||
| Bulge|| "circumferential symmetric extension of the disk beyond the interspace (around the end plates)"||52% | |||
|- | |||
| Protrusion||"focal or asymmetric extension of the disk beyond the interspace, with the base against the disk of origin broader than any other dimension of the protrusion" ||27% | |||
|- | |||
| Extrusion||"more extreme extension of the disk beyond the interspace, with the base against the disk of origin narrower than the diameter of the extruding material itself or with no connection between the material and the disk of origin" ||1% | |||
|} | |||
==Diagnosis== | ==Diagnosis== | ||
===History and physical examination=== | ===History and physical examination=== | ||
{| class="wikitable" | |||
|+ Diagnosis of herniated lumbar herniated disk.<ref name="pmid20166095">{{cite journal| author=van der Windt DA, Simons E, Riphagen II, Ammendolia C, Verhagen AP, Laslett M et al.| title=Physical examination for lumbar radiculopathy due to disc herniation in patients with low-back pain. | journal=Cochrane Database Syst Rev | year= 2010 | volume= 2 | issue= | pages= CD007431 | pmid=20166095 | |||
| url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=clinical.uthscsa.edu/cite&retmode=ref&cmd=prlinks&id=20166095 | doi=10.1002/14651858.CD007431.pub2 }} </ref><ref name="pmid1386391">{{cite journal |author=Deyo RA, Rainville J, Kent DL |title=What | |||
can the history and physical examination tell us about low back pain? |journal=JAMA |volume=268 |issue=6 | |||
|pages=760–5 |year=1992 |pmid=1386391 |doi= |issn=}}</ref> | |||
! Finding!! [[Sensitivity and specificity|Sensitivity]]!! [[Sensitivity and specificity|Specificity]] | |||
|- | |||
| [[Sciatica]]|| 95%<ref name="pmid1386391"/>|| 88%<ref name="pmid1386391"/> | |||
|- | |||
| [[Straight leg raise]]|| 92%<ref name="pmid20166095"/> to 80%<ref name="pmid1386391"/>|| 28%<ref name="pmid20166095"/> to 40%<ref name="pmid1386391"/> | |||
|- | |||
| Crossed [[straight leg raise]]|| 28%<ref name="pmid20166095"/>|| 95%<ref name="pmid20166095"/> | |||
|} | |||
===Testing=== | |||
The role of [[magnetic resonance imaging]] is not clear.<ref name="pmid22157067">{{cite journal| author=Cohen SP, Gupta A, Strassels SA, Christo PJ, Erdek MA, Griffith SR et al.| title=Effect of MRI on treatment results or decision making in patients with lumbosacral radiculopathy referred for epidural steroid injections: a multicenter, randomized controlled trial. | journal=Arch Intern Med | year= 2012 | volume= 172 | issue= 2 | pages= 134-42 | pmid=22157067 | doi=10.1001/archinternmed.2011.593 | pmc= | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=22157067 }} </ref> | |||
==Treatment== | ==Treatment== | ||
[[Randomized controlled trial]]s address discectomy (diskectomy) versus conservative care.<ref name="pmid17443505">{{cite journal |author=Gibson JN, Waddell G |title=Surgical interventions for lumbar disc prolapse |journal=Cochrane Database Syst Rev |volume= |issue=2 |pages=CD001350 |year=2007 |pmid=17443505 |doi=10.1002/14651858.CD001350.pub4 |url=http://dx.doi.org/10.1002/14651858.CD001350.pub4 |issn=}}</ref> Microdiskectomy (with a microscope or loupe magnification) and open diskectomy are comparable according to a [[systematic review]] by the [[Cochrane Collaboration]].<ref name="pmid17443505"/> | |||
The Spine Patient Outcomes Research Trial (SPORT) of 501 patients receiving an unstated mix of surgical procedures found "patients in both the surgery and the nonoperative treatment groups improved substantially over a 2-year period. Because of the large numbers of patients who crossed over in both directions, conclusions about the superiority or equivalence of the treatments are not warranted based on the intent-to-treat analysis."<ref name="pmid17119140">{{cite journal |author=Weinstein JN, Tosteson TD, Lurie JD, ''et al'' |title=Surgical vs nonoperative treatment for lumbar disk herniation: the Spine Patient Outcomes Research Trial (SPORT): a randomized trial |journal=JAMA : the journal of the American Medical Association |volume=296 |issue=20 |pages=2441–50 |year=2006 |month=November |pmid=17119140 |pmc=2553805 |doi=10.1001/jama.296.20.2441 |url=http://jama.ama-assn.org/cgi/pmidlookup?view=long&pmid=17119140 |issn=}}</ref><ref name="pmid17119141">{{cite journal |author=Weinstein JN, Lurie JD, Tosteson TD, ''et al'' |title=Surgical vs nonoperative treatment for lumbar disk herniation: the Spine Patient Outcomes Research Trial (SPORT) observational cohort |journal=JAMA : the journal of the American Medical Association |volume=296 |issue=20 |pages=2451–9 |year=2006 |month=November |pmid=17119141 |pmc=2562254 |doi=10.1001/jama.296.20.2451 |url=http://jama.ama-assn.org/cgi/pmidlookup?view=long&pmid=17119141 |issn=}}</ref> The costs may be acceptable.<ref name="pmid18777603">{{cite journal |author=Tosteson AN, Skinner JS, Tosteson TD, ''et al'' |title=The cost effectiveness of surgical versus nonoperative treatment for lumbar disc herniation over two years: evidence from the Spine Patient Outcomes Research Trial (SPORT) |journal=Spine |volume=33 |issue=19 |pages=2108–15 |year=2008 |month=September |pmid=18777603 |doi= |url= |issn=}}</ref> | |||
===Surgery=== | |||
Timing of surgery. | |||
Surgical results in a [[randomized controlled trial]] are better if surgery occurs within six months of the onset of symptoms; however, "The relative increased benefit of surgery compared with nonoperative treatment was not dependent on the duration of the symptoms."<ref name="pmid22012528">{{cite journal| author=Rihn JA, Hilibrand AS, Radcliff K, Kurd M, Lurie J, Blood E et al.| title=Duration of Symptoms Resulting from Lumbar Disc Herniation: Effect on Treatment Outcomes: Analysis of the Spine Patient Outcomes Research Trial (SPORT). | journal=J Bone Joint Surg Am | year= 2011 | volume= 93 | issue= 20 | pages= 1906-14 | pmid=22012528 | doi=10.2106/JBJS.J.00878 | pmc= | url= }} </ref> | |||
Regarding quicker surgery at 6 weeks, a subgroup analysis of a previous trial found "Early surgery resulted in a faster recovery of motor deficit accompanying sciatica compared with prolonged conservative treatment but the difference was no longer significant during the final follow-up examination at 1 year."<ref name="pmid24200407">{{cite journal| author=Overdevest GM, Vleggeert-Lankamp CL, Jacobs WC, Brand R, Koes BW, Peul WC et al.| title=Recovery of motor deficit accompanying sciatica-subgroup analysis of a randomized controlled trial. | journal=Spine J | year= 2013 | volume= | issue= | pages= | pmid=24200407 | doi=10.1016/j.spinee.2013.07.456 | pmc= | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=24200407 }} </ref> | |||
====Microdiskectomy==== | |||
Microdiskectomy uses unilateral transflaval approach with magnification provided by either a microscope or loupe. Some authors do not consider loupe magnification to be microdiskectomy. The Leiden-The Hague Spine Intervention Prognostic Study of 283 patients found that microdiskectomy led to quicker improvement at one year<ref name="pmid17538084">{{cite journal |author=Peul WC, van Houwelingen HC, van den Hout WB, ''et al'' |title=Surgery versus prolonged conservative treatment for sciatica |journal=The New England journal of medicine |volume=356 |issue=22 |pages=2245–56 |year=2007 |month=May |pmid=17538084 |doi=10.1056/NEJMoa064039 |url=http://content.nejm.org/cgi/pmidlookup?view=short&pmid=17538084&promo=ONFLNS19 |issn=}}</ref>, with no further changes after two years.<ref>Peul WC, Hout WB, Brand R, Thomeer RT, Koes BW; for the Leiden-The Hague Spine Intervention Prognostic Study Group. Prolonged conservative care versus early surgery in patients with sciatica caused by lumbar disc herniation: two year results of a randomised controlled trial. BMJ. 2008 May 23. PMID 18502911</ref> The cost of surgery might be acceptable to some patients.<ref>Hout WB, Peul WC, Koes BW, Brand R, Kievit J, Thomeer RT; for the Leiden-The Hague Spine Intervention Prognostic Study Group. Prolonged conservative care versus early surgery in patients with sciatica from lumbar disc herniation: cost utility analysis alongside a randomised controlled trial. BMJ. 2008 May 23. PMID 18502912</ref> | |||
====Open diskectomy==== | |||
The open diskectomy uses unilateral transflaval approach without magnification. | |||
==Prognosis== | |||
The presence of a herniated disk (protrusion or extrusion) does not affect the prognosis of low back pain.<ref name="pmid23484826">{{cite journal| author=el Barzouhi A, Vleggeert-Lankamp CL, Lycklama à Nijeholt GJ, Van der Kallen BF, van den Hout WB, Jacobs WC et al.| title=Magnetic resonance imaging in follow-up assessment of sciatica. | journal=N Engl J Med | year= 2013 | volume= 368 | issue= 11 | pages= 999-1007 | pmid=23484826 | doi=10.1056/NEJMoa1209250 | pmc= | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=23484826 }} </ref> | |||
==References== | ==References== | ||
{{reflist}}[[Category:Suggestion Bot Tag]] | |||
[[Category: | |||
Latest revision as of 11:00, 27 August 2024
In medicine, a herniated disk is defined as an "intervertebral disk in which the nucleus pulposus has protruded through surrounding fibrocartilage. This occurs most frequently in the lower lumbar region.".[1]
A herniated disk is an infrequent, but important cause of low back pain. A herniated disk is more likely when sciatica is present.
Epidemiology
| Abnormality | Definition | Prevalence |
|---|---|---|
| Bulge | "circumferential symmetric extension of the disk beyond the interspace (around the end plates)" | 52% |
| Protrusion | "focal or asymmetric extension of the disk beyond the interspace, with the base against the disk of origin broader than any other dimension of the protrusion" | 27% |
| Extrusion | "more extreme extension of the disk beyond the interspace, with the base against the disk of origin narrower than the diameter of the extruding material itself or with no connection between the material and the disk of origin" | 1% |
Diagnosis
History and physical examination
| Finding | Sensitivity | Specificity |
|---|---|---|
| Sciatica | 95%[4] | 88%[4] |
| Straight leg raise | 92%[3] to 80%[4] | 28%[3] to 40%[4] |
| Crossed straight leg raise | 28%[3] | 95%[3] |
Testing
The role of magnetic resonance imaging is not clear.[5]
Treatment
Randomized controlled trials address discectomy (diskectomy) versus conservative care.[6] Microdiskectomy (with a microscope or loupe magnification) and open diskectomy are comparable according to a systematic review by the Cochrane Collaboration.[6]
The Spine Patient Outcomes Research Trial (SPORT) of 501 patients receiving an unstated mix of surgical procedures found "patients in both the surgery and the nonoperative treatment groups improved substantially over a 2-year period. Because of the large numbers of patients who crossed over in both directions, conclusions about the superiority or equivalence of the treatments are not warranted based on the intent-to-treat analysis."[7][8] The costs may be acceptable.[9]
Surgery
Timing of surgery. Surgical results in a randomized controlled trial are better if surgery occurs within six months of the onset of symptoms; however, "The relative increased benefit of surgery compared with nonoperative treatment was not dependent on the duration of the symptoms."[10]
Regarding quicker surgery at 6 weeks, a subgroup analysis of a previous trial found "Early surgery resulted in a faster recovery of motor deficit accompanying sciatica compared with prolonged conservative treatment but the difference was no longer significant during the final follow-up examination at 1 year."[11]
Microdiskectomy
Microdiskectomy uses unilateral transflaval approach with magnification provided by either a microscope or loupe. Some authors do not consider loupe magnification to be microdiskectomy. The Leiden-The Hague Spine Intervention Prognostic Study of 283 patients found that microdiskectomy led to quicker improvement at one year[12], with no further changes after two years.[13] The cost of surgery might be acceptable to some patients.[14]
Open diskectomy
The open diskectomy uses unilateral transflaval approach without magnification.
Prognosis
The presence of a herniated disk (protrusion or extrusion) does not affect the prognosis of low back pain.[15]
References
- ↑ National Library of Medicine. Intervertebral Disk Displacement. Retrieved on 2007-11-13.
- ↑ Jensen MC, Brant-Zawadzki MN, Obuchowski N, Modic MT, Malkasian D, Ross JS (1994). "Magnetic resonance imaging of the lumbar spine in people without back pain.". N Engl J Med 331 (2): 69-73. DOI:10.1056/NEJM199407143310201. PMID 8208267. Research Blogging.
- ↑ 3.0 3.1 3.2 3.3 3.4 van der Windt DA, Simons E, Riphagen II, Ammendolia C, Verhagen AP, Laslett M et al. (2010). "Physical examination for lumbar radiculopathy due to disc herniation in patients with low-back pain.". Cochrane Database Syst Rev 2: CD007431. DOI:10.1002/14651858.CD007431.pub2. PMID 20166095. Research Blogging.
- ↑ 4.0 4.1 4.2 4.3 4.4 Deyo RA, Rainville J, Kent DL (1992). "What can the history and physical examination tell us about low back pain?". JAMA 268 (6): 760–5. PMID 1386391. [e]
- ↑ Cohen SP, Gupta A, Strassels SA, Christo PJ, Erdek MA, Griffith SR et al. (2012). "Effect of MRI on treatment results or decision making in patients with lumbosacral radiculopathy referred for epidural steroid injections: a multicenter, randomized controlled trial.". Arch Intern Med 172 (2): 134-42. DOI:10.1001/archinternmed.2011.593. PMID 22157067. Research Blogging.
- ↑ 6.0 6.1 Gibson JN, Waddell G (2007). "Surgical interventions for lumbar disc prolapse". Cochrane Database Syst Rev (2): CD001350. DOI:10.1002/14651858.CD001350.pub4. PMID 17443505. Research Blogging.
- ↑ Weinstein JN, Tosteson TD, Lurie JD, et al (November 2006). "Surgical vs nonoperative treatment for lumbar disk herniation: the Spine Patient Outcomes Research Trial (SPORT): a randomized trial". JAMA : the journal of the American Medical Association 296 (20): 2441–50. DOI:10.1001/jama.296.20.2441. PMID 17119140. PMC 2553805. Research Blogging.
- ↑ Weinstein JN, Lurie JD, Tosteson TD, et al (November 2006). "Surgical vs nonoperative treatment for lumbar disk herniation: the Spine Patient Outcomes Research Trial (SPORT) observational cohort". JAMA : the journal of the American Medical Association 296 (20): 2451–9. DOI:10.1001/jama.296.20.2451. PMID 17119141. PMC 2562254. Research Blogging.
- ↑ Tosteson AN, Skinner JS, Tosteson TD, et al (September 2008). "The cost effectiveness of surgical versus nonoperative treatment for lumbar disc herniation over two years: evidence from the Spine Patient Outcomes Research Trial (SPORT)". Spine 33 (19): 2108–15. PMID 18777603. [e]
- ↑ Rihn JA, Hilibrand AS, Radcliff K, Kurd M, Lurie J, Blood E et al. (2011). "Duration of Symptoms Resulting from Lumbar Disc Herniation: Effect on Treatment Outcomes: Analysis of the Spine Patient Outcomes Research Trial (SPORT).". J Bone Joint Surg Am 93 (20): 1906-14. DOI:10.2106/JBJS.J.00878. PMID 22012528. Research Blogging.
- ↑ Overdevest GM, Vleggeert-Lankamp CL, Jacobs WC, Brand R, Koes BW, Peul WC et al. (2013). "Recovery of motor deficit accompanying sciatica-subgroup analysis of a randomized controlled trial.". Spine J. DOI:10.1016/j.spinee.2013.07.456. PMID 24200407. Research Blogging.
- ↑ Peul WC, van Houwelingen HC, van den Hout WB, et al (May 2007). "Surgery versus prolonged conservative treatment for sciatica". The New England journal of medicine 356 (22): 2245–56. DOI:10.1056/NEJMoa064039. PMID 17538084. Research Blogging.
- ↑ Peul WC, Hout WB, Brand R, Thomeer RT, Koes BW; for the Leiden-The Hague Spine Intervention Prognostic Study Group. Prolonged conservative care versus early surgery in patients with sciatica caused by lumbar disc herniation: two year results of a randomised controlled trial. BMJ. 2008 May 23. PMID 18502911
- ↑ Hout WB, Peul WC, Koes BW, Brand R, Kievit J, Thomeer RT; for the Leiden-The Hague Spine Intervention Prognostic Study Group. Prolonged conservative care versus early surgery in patients with sciatica from lumbar disc herniation: cost utility analysis alongside a randomised controlled trial. BMJ. 2008 May 23. PMID 18502912
- ↑ el Barzouhi A, Vleggeert-Lankamp CL, Lycklama à Nijeholt GJ, Van der Kallen BF, van den Hout WB, Jacobs WC et al. (2013). "Magnetic resonance imaging in follow-up assessment of sciatica.". N Engl J Med 368 (11): 999-1007. DOI:10.1056/NEJMoa1209250. PMID 23484826. Research Blogging.